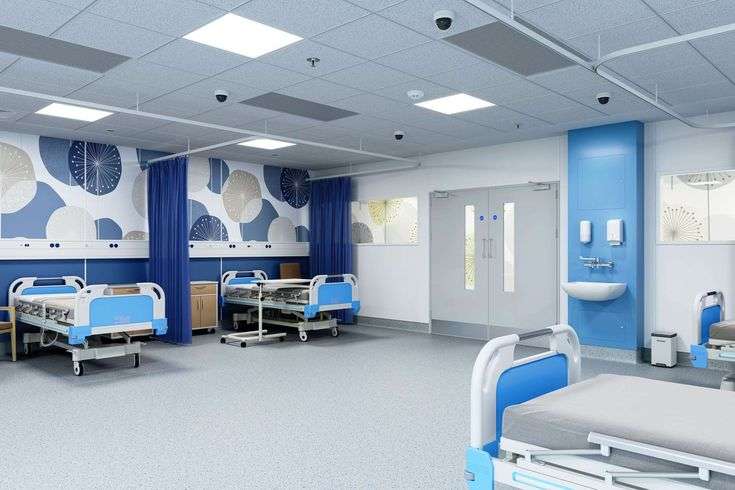
Building a Hospital: How Much Money Do You Really Need?
February 20, 2026Why Hospital Renovation Is Never Just About Bricks and Paint
Renovating an old hospital sounds straightforward on paper. You upgrade spaces, modernize infrastructure, improve safety, and move on. But anyone who’s actually stood inside a working hospital knows that it’s never that simple. Patients don’t stop arriving just because scaffolding goes up. Doctors don’t pause surgeries because tiles are being replaced. Life, quite literally, continues.
That’s what makes Hospital renovation different from almost every other type of renovation. You’re not just working around furniture or office hours. You’re working around pain, recovery, emergencies, and sometimes fear. And that reality should shape every decision, from planning to execution.
Understanding the Real Stakes Before You Start
Before the first wall is opened or the first contractor steps in, there’s an uncomfortable question that needs answering: What happens if something goes wrong?
In a hospital, “wrong” doesn’t mean delays or budget overruns alone. It can mean noise disturbing a patient who hasn’t slept in two days. It can mean dust affecting someone with respiratory issues. It can mean confusion during an emergency because a corridor layout changed overnight.
Renovation in this environment isn’t just technical. It’s deeply human.
Start With Phased Planning, Not Big-Bang Changes
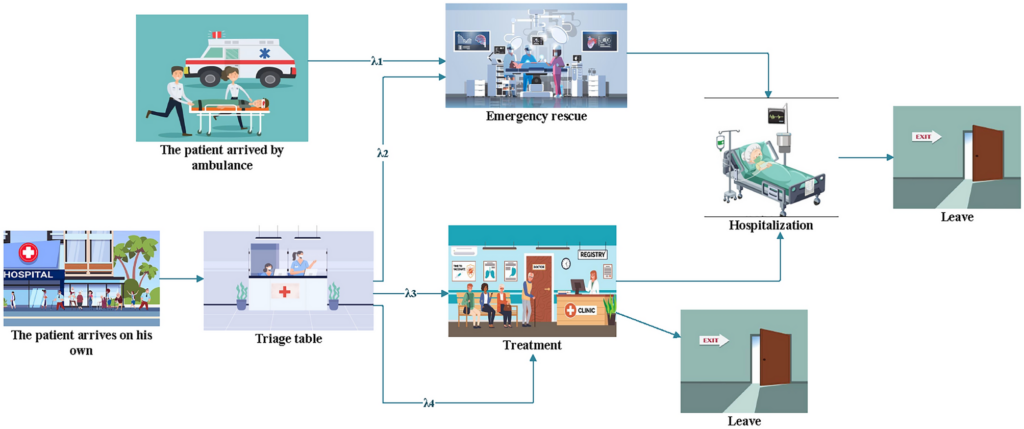
Trying to do too much at once is one of the most frequent mistakes made when renovating a hospital. On paper, it seems efficient—complete more quickly, cut costs overall, and move on. In practice, it’s frequently chaotic.
A phased approach is more effective. The hospital is divided into zones, and each one is renovated while the others remain open. It’s slower, yes. But it’s controlled.
Phasing allows teams to:
- Maintain uninterrupted patient services
- Shift departments temporarily without panic
- Adjust plans based on what’s working (and what’s not)
And that flexibility matters more than speed in a live healthcare environment.
Temporary Relocation Isn’t a Failure, It’s a Strategy
There’s a strange reluctance some hospitals have around temporary relocation. As if moving a department—even briefly—means admitting defeat. It doesn’t.
Smart renovations plan temporary shifts intentionally. OPDs might move to modular setups. Diagnostics might operate in extended hours elsewhere. Even inpatient wards can be relocated floor-by-floor with careful coordination.
The goal isn’t to avoid movement. It’s to control it.
Communication Is as Important as Construction
This part gets underestimated constantly.
Even with the greatest architects and most skilled contractors, disruptions will still occur if physicians, nurses, and support personnel are not properly informed. Confusion creates stress. Stress spreads fast in hospitals.
Clear communication should include:
- Renovation timelines shared well in advance
- Daily or weekly updates for affected departments
- Signage that’s simple and impossible to ignore
Patients don’t need technical details. They need reassurance. Staff need predictability. Both are non-negotiable.
Noise, Dust, and Smell Are Silent Disruptors
Renovation isn’t just visually disruptive. Noise, dust, and even chemical smells can affect recovery, sleep, and staff performance. These aren’t minor issues—they’re clinical ones.
Simple mitigation measures go a long way:
- Night-time or off-peak noisy work
- Proper sealing of renovation zones
- Negative air pressure in construction areas
- Frequent cleaning beyond normal schedules
These steps don’t make renovation invisible. But they make it tolerable.
Infection Control Must Lead Every Decision
Older hospitals weren’t designed with modern infection control standards in mind. Renovation is the perfect opportunity to correct that—but also the riskiest moment if done poorly.
Increased foot traffic, open ceilings, and construction dust can all increase the risk of infection. Increased foot traffic, open ceilings, and construction dust can all increase the risk of infection. Coordination between the renovation and clinical teams becomes crucial at this point.
It is not appropriate for infection control procedures to be a checklist item or an afterthought. They ought to direct worker movement within the building as well as scheduling and material usage.
Technology Upgrades Without System Downtime
Upgrading the electrical, HVAC, medical gas, and IT infrastructure is nearly always necessary when plannning to go for hospital renovation. Upgrading them isn’t the problem. It’s accomplishing this without shutting them down.
Planning for redundancy is crucial. Risk is decreased by staged cutovers, backup power, and temporary systems. Nothing should go offline without a safety net already in place.
This is one area where over-planning isn’t a waste. It’s protection.
Respect the Emotional Side of Care Spaces
Hospitals carry emotional weight. A ward isn’t just a room. It’s where someone waited for news. Where families held their breath. Where lives changed.
Renovation teams sometimes overlook this softer side. But patients and families don’t. Anxiety can be exacerbated by abrupt visual changes, obscured views, or strange layouts.
Design decisions should strive for familiarity rather than surprise. Even if the ultimate objective is the same, gradual change seems safer than drastic transformation.
Train Staff Before the Space Changes
Staff orientation is one of the most neglected phases in hospital renovation. Workflows are altered by renovations, sometimes in subtle ways and other times in significant ways.
Before reopening a renovated area:
- Walk staff through new layouts
- Explain changes in patient flow
- Test emergency scenarios
Confidence reduces disruption. Confusion multiplies it.
Measure Impact, Not Just Completion
Finishing renovation doesn’t mean it worked.
Did patient wait times increase?
Did staff movement become easier—or harder?
Did noise complaints drop?
Post-renovation evaluation matters. It helps hospitals learn, adjust, and prepare better for future upgrades. Renovation should be a process of improvement, not just construction.
When Experience Matters More Than Speed
There’s a temptation to treat renovation as a race. Finish faster. Reopen sooner. Celebrate.
But hospitals don’t benefit from rushed change. They benefit from thoughtful, measured progress. Experience matters—especially experience that understands both construction realities and healthcare realities.
Professional hospital renovation services can have a significant impact in this situation. They plan better, foresee risks, and respect the environment they work in—not because they build things faster.
The Renovation Is Temporary. Care Is Permanent.
Schedules, budgets, and drawings can easily cause one to lose focus. However, the sole purpose of Hospital consultation is to provide care. Instead of competing with that goal, renovation should serve it.
The renovations that patients hardly remember are the best. where the care went on. where employees adjusted without becoming burned out. where progress felt organic rather than coerced.
Aesthetics are not the only factor in selecting the best hospital renovation services. It’s about preserving continuity, dignity, and trust—things that are far more important than fixtures and finishes.
Final Thought
It’s challenging to renovate an old hospital while maintaining full functionality. It calls for tolerance, modesty, and regard for the area and its occupants. However, when done carefully, it strengthens care itself rather than merely enhancing infrastructure.
And even if it takes a little longer, doing it correctly is worthwhile.